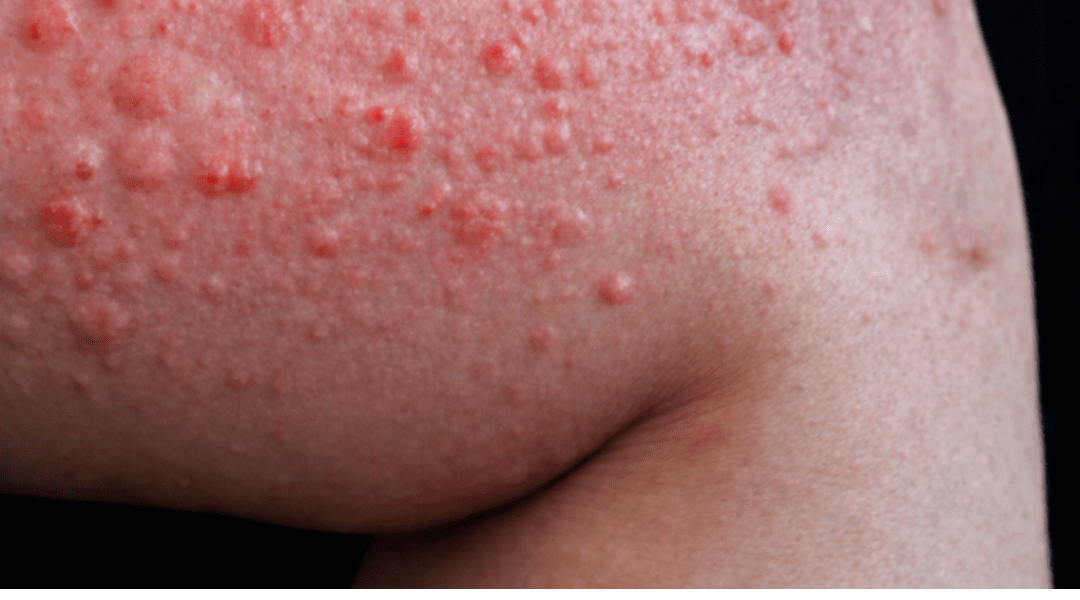
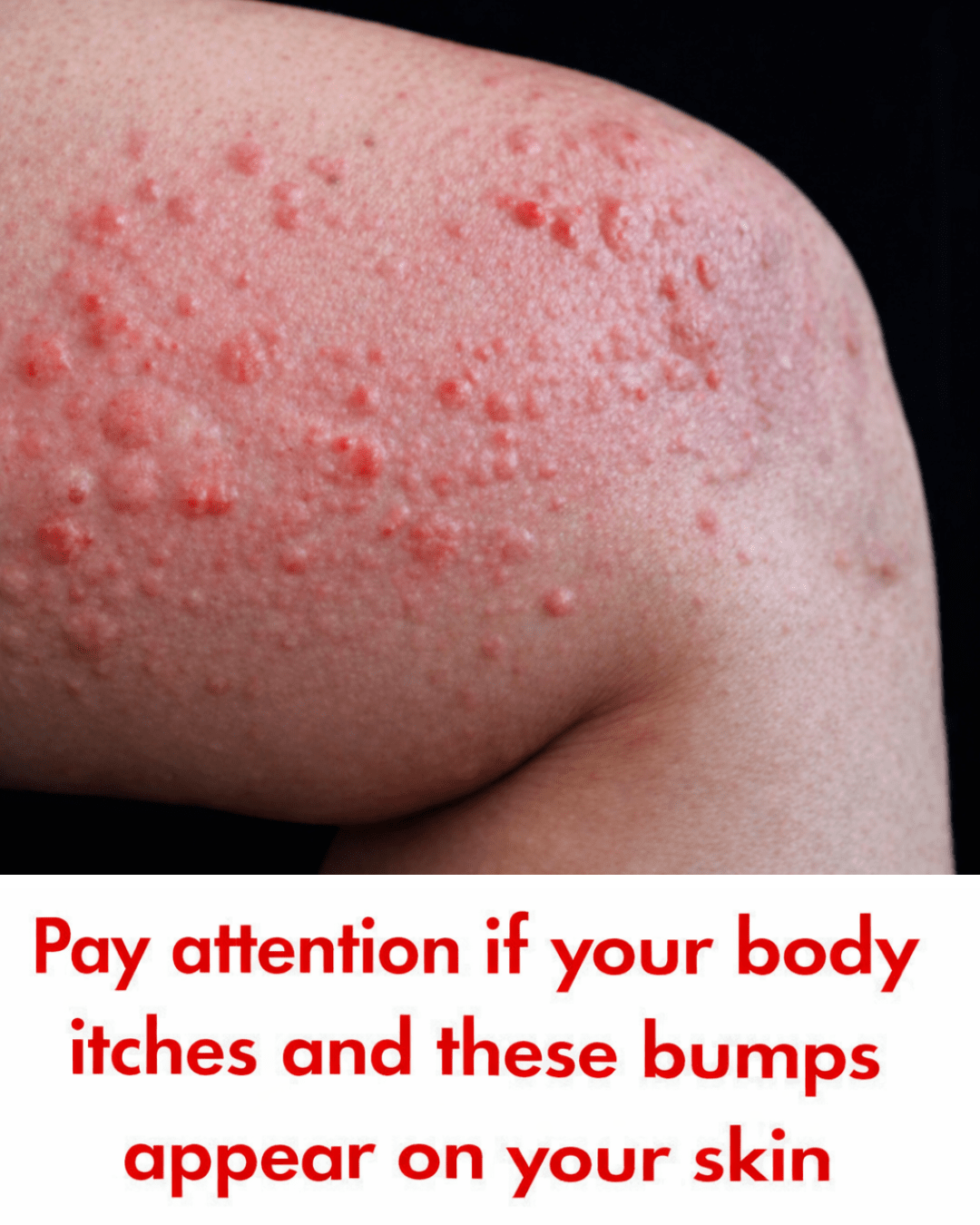
Imagine waking up to find red, itchy welts covering your arms, legs, or torso — hives that sting, burn, and make even loose clothing feel unbearable. These raised patches can swell dramatically, shift locations throughout the day, and leave you scratching relentlessly, disrupting sleep and daily life. The frustration builds when hives appear without warning, turning simple moments into constant discomfort and self-consciousness. But understanding the hidden triggers behind hives can empower you to reduce outbreaks — and there’s one surprising factor many people completely overlook that might be fueling your flares more than you realize.
😩 What Exactly Are Hives and What’s Happening Beneath Your Skin?
Hives, also known as urticaria, are your body’s way of sounding an alarm when something irritates it. Mast cells in the skin release histamine, causing blood vessels to widen and leak fluid into surrounding tissues. This creates those signature red, swollen welts we recognize as hives — often intensely itchy and unpredictable.
The discomfort from hives can feel overwhelming, making concentration difficult and social situations embarrassing. Research shows this reaction is remarkably consistent across triggers, which is why identifying patterns matters so much for managing hives effectively.
But here’s the thing: not all hives behave the same way.
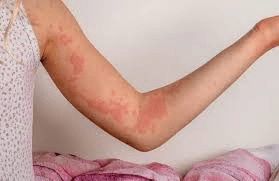
🩺 Acute vs. Chronic Hives: Understanding the Difference
Acute hives typically resolve within six weeks and often link to an identifiable cause. They strike suddenly but usually fade quickly once the trigger is removed.
Chronic hives, however, persist longer than six weeks and can recur for months or years. In many cases, no obvious cause is found — what experts call chronic spontaneous urticaria. Studies, including those from the Mayo Clinic, suggest autoimmune factors may play a role in up to half of chronic hives cases, where the immune system mistakenly keeps mast cells on high alert.
Living with chronic hives adds ongoing stress and uncertainty, as outbreaks seem random and relentless. The good news? Tracking patterns can still reveal clues, even in chronic hives.
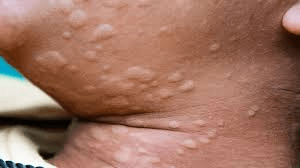
🍤 Common Triggers for Hives Most People Recognize
Many hives episodes stem from familiar sources that are relatively straightforward to spot:
- Certain foods like shellfish, nuts, eggs, or dairy
- Medications, especially NSAIDs or antibiotics
- Insect bites or stings
- Viral infections, such as colds or flu
These classic triggers often cause acute hives and resolve once exposure ends. According to WebMD, food reactions and medications top the list for short-term hives outbreaks.
Yet for many sufferers, avoiding these obvious culprits doesn’t stop hives from returning. That’s where lesser-known triggers come in.
😲 Surprising Triggers for Hives You Might Be Overlooking
The surprising part is how everyday physical and emotional factors can spark hives without any allergic involvement. Here are some common but often missed triggers:
- Stress and anxiety — Emotional tension sensitizes mast cells, amplifying histamine release and worsening hives intensity
- Pressure on the skin — Tight clothing, backpack straps, or even sitting on a hard surface
- Temperature changes — Extreme heat, cold, sweating, or hot showers
- Friction or scratching — Known as dermatographism, where light stroking raises welts within minutes
- Sun exposure — Intense sunlight can provoke hives in sensitive individuals
- Exercise — Physical exertion sometimes triggers cholinergic hives through sweating
The American Academy of Dermatology notes that physical stimuli like these account for many inducible hives cases. Dermatographism alone affects 2-5% of people and is one of the most under-recognized forms of hives.
And that’s not all — even water contact or vibrations can rarely trigger hives in specific types.
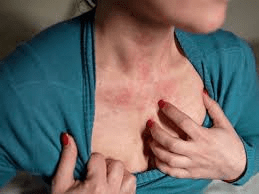
🧘 The Hidden Role Stress Plays in Fueling Hives
Stress doesn’t usually cause hives on its own, but it acts as a powerful amplifier. When you’re anxious or overwhelmed, your body releases chemicals that make mast cells more reactive to other triggers.
Research links higher stress levels to increased frequency and severity of hives outbreaks. For those with chronic hives, daily pressures can keep the cycle going, turning occasional flares into regular battles.
The emotional toll compounds the physical itching — feeling trapped in your own skin during stressful periods. Simple relaxation practices can help break this loop and reduce hives episodes.
🩹 Practical Steps to Calm Hives and Prevent Future Outbreaks
While hives often resolve on their own, these evidence-based strategies can speed relief and lower recurrence:
- Take non-drowsy antihistamines like cetirizine, loratadine, or fexofenadine as soon as hives appear — they block histamine and usually ease symptoms within hours
- Apply cool compresses or take lukewarm oatmeal baths to soothe itching and reduce swelling
- Wear loose, breathable clothing and avoid hot showers or harsh soaps
- Keep a simple trigger journal noting foods, activities, weather, and stress levels to spot patterns over time
- Practice stress-reduction techniques like deep breathing, gentle exercise, or mindfulness
Dermatologists recommend starting with second-generation antihistamines for daily management of persistent hives. Consistency often brings noticeable improvement.
🚨 When Hives Require Professional Medical Attention
Most hives are harmless and self-limiting, but certain signs warrant prompt evaluation:
- Outbreaks lasting more than six weeks
- Frequent recurrence disrupting daily life
- Swelling of lips, eyelids, throat, or tongue (possible angioedema)
- Accompanying symptoms like difficulty breathing, dizziness, or abdominal pain
These could indicate a more serious reaction needing immediate care.
Final Thoughts: Taking Back Control from Hives
Hives on your skin send a clear message that something is triggering your body’s defense system — whether obvious allergies or hidden factors like stress and physical pressure. By recognizing both common and surprising triggers for hives, acting quickly with proven strategies, and monitoring patterns, many people significantly reduce outbreaks and regain comfort in their skin.
Your body is trying to communicate. Listening closely can minimize the itching, burning, and frustration that hives bring.
Frequently Asked Questions About Hives
Can stress alone cause hives to appear?
Stress rarely acts as the sole trigger but strongly amplifies other factors, making mast cells more reactive and increasing hives likelihood during tense periods.
Are hives contagious?
No, hives are not contagious. They result from internal reactions rather than bacteria or viruses that spread person-to-person.
Do children experience the same hives triggers as adults?
Children often develop hives from viral infections or new foods, while physical triggers and stress become more prominent in adults. Most childhood cases remain mild and temporary.
Disclaimer: This article is for informational purposes only and is not intended to diagnose, treat, or cure any medical condition. Always consult a qualified healthcare professional for personalized medical advice regarding hives or any skin concerns.