Rheumatoid arthritis (RA) can bring persistent joint pain, morning stiffness, and fatigue that make everyday activities—like opening jars, walking comfortably, or simply getting out of bed—feel challenging and draining. These symptoms often linger despite rest, impacting energy, mood, and independence in ways that feel deeply frustrating. Yet ongoing research and treatment options, including medications and supportive strategies, may help many people achieve better control over inflammation and daily comfort.
What if staying informed about established and emerging approaches could open doors to improved quality of life? Keep reading for practical insights backed by medical guidelines and recent studies.
🩺 Understanding Rheumatoid Arthritis and Its Daily Impact
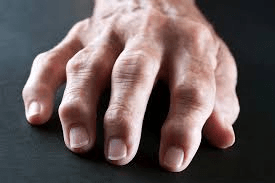
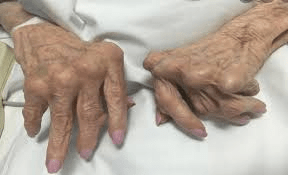
Rheumatoid arthritis is an autoimmune condition where the immune system mistakenly attacks joint linings, leading to inflammation, swelling, and potential damage over time. According to the American College of Rheumatology (ACR), early and consistent management is key to slowing progression.
For many, this means dealing with flares that disrupt plans, alongside ongoing tiredness. Research shows that targeted treatments can reduce these effects, helping maintain mobility and function.
🔬 Established Treatments That Form the Foundation of RA Care
Guidelines from the ACR emphasize starting with disease-modifying antirheumatic drugs (DMARDs) to address underlying inflammation.
- Methotrexate: Often the first-line choice, it may slow disease progression effectively for many.
- Other Conventional DMARDs: Options like leflunomide or sulfasalazine provide alternatives when needed.
- Biologic DMARDs: TNF inhibitors (e.g., etanercept, adalimumab) or IL-6 blockers (e.g., tocilizumab) target specific immune pathways.
- JAK Inhibitors: Oral medications like tofacitinib or upadacitinib offer convenient options for moderate to severe cases.
These approaches, often used in combination, help many achieve low disease activity.
🌟 Recent Advances Bringing New Options to RA Management
Medical research continues to evolve, with several developments noted in recent years:
- Biosimilars: More affordable versions of biologics, increasing access to proven therapies.
- Vagus Nerve Stimulation: A non-invasive device approved in 2025 that may help reduce inflammation through nerve signals.
- Preventive Approaches: Studies suggest abatacept may delay RA onset in high-risk individuals.
- GLP-1 Agonists: Emerging data indicates these diabetes/obesity medications might reduce flares in some patients.
- Experimental Therapies: Compounds like rosnilimab show promise in early trials for targeting overactive immune cells.
These advances highlight ongoing efforts to refine and expand RA care.
❤️ Personal Experiences with RA Management
Many individuals share how combining treatments with lifestyle adjustments has made a difference.
Jane, 55, found that adding a JAK inhibitor to methotrexate reduced her morning stiffness significantly, allowing more active days.
Mark, 62, benefited from physical therapy alongside biologics, regaining confidence in hobbies like gardening.
While experiences vary, consistent care often supports better outcomes.
🥦 Supportive Strategies to Complement Medical Treatments
Beyond medications, evidence-based habits may enhance well-being:

- Anti-Inflammatory Eating: A Mediterranean-style diet rich in fruits, vegetables, and omega-3s.
- Regular Gentle Exercise: Low-impact activities like swimming or walking to maintain joint flexibility.
- Stress Reduction: Techniques such as mindfulness or yoga, linked to fewer flares in studies.
- Adequate Sleep: Prioritizing rest to combat fatigue.
- Joint Protection: Using ergonomic tools and pacing activities.
📊 Comparing Common RA Treatment Approaches
| Treatment Type | Examples | Potential Benefits | Considerations |
|---|---|---|---|
| Conventional DMARDs | Methotrexate, hydroxychloroquine | Slows progression, oral convenience | Regular monitoring needed |
| Biologics & Biosimilars | Adalimumab, tocilizumab | Targeted action, effective for many | Injection/infusion, infection risk |
| JAK Inhibitors | Upadacitinib, tofacitinib | Oral, rapid relief possible | Blood tests for safety |
| Emerging Non-Drug | Vagus nerve device | Non-invasive inflammation support | Availability and suitability vary |
| Lifestyle Supports | Diet, exercise | Overall wellness, no side effects | Requires consistency |
🚀 Practical Steps to Discuss with Your Doctor
- Review current symptoms and treatment response.
- Ask about recent options like biosimilars or new devices.
- Explore combining therapies for better control.
- Incorporate supportive habits gradually.
- Schedule regular monitoring for adjustments.
Early and personalized plans often yield the strongest results.
Conclusion: Progress and Possibilities in RA Care
Advances in rheumatoid arthritis treatments—from refined medications to innovative devices and preventive strategies—offer meaningful support for managing symptoms and protecting joints. Working closely with a rheumatologist helps tailor approaches to individual needs.
Small, informed steps today can contribute to more comfortable tomorrows.

Frequently Asked Questions
When should I start treatment for RA?
Early intervention is recommended—guidelines suggest beginning DMARDs soon after diagnosis to help preserve joint health.
Are new treatments like vagus nerve stimulation suitable for everyone?
Suitability varies; discuss with your healthcare provider to weigh benefits and access.
Can lifestyle changes really help with RA symptoms?
Research supports that anti-inflammatory diets and exercise may complement medications by reducing flares and improving function.
This article is for informational purposes only and is not medical advice. Rheumatoid arthritis management requires professional guidance—always consult your rheumatologist or healthcare provider for personalized recommendations, monitoring, and treatment decisions. Regular assessments remain essential.